GUEST BLOG: X-ing Out the J-Curve
Three Big Questions About the Global Burden of Disease Project’s Findings on Alcohol by Carson Benowitz-Fredericks, MSPH
by Carson Benowitz-Fredericks, MSPH
Research Manager, Alcohol Justice
Last month, The Lancet published a powerful study online ahead of print examining the use and harms of alcohol on a global scale. The study, part of the Bill and Melinda Gates Foundation-sponsored Global Burden of Disease (GBD) project, casts a startling spotlight on the ways alcohol impacts each 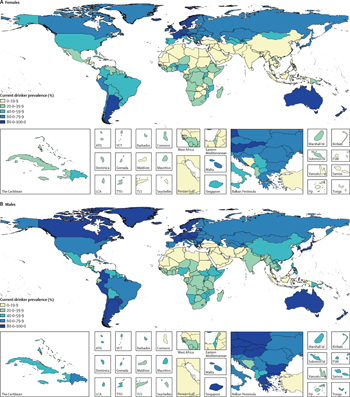 country differently, yet hits everyone across the globe. The study was heavily covered primarily for how it debunks Big Alcohol’s pet dissemblance surrounding “healthy alcohol”. As significant as that finding is, however, the significance of the GBD findings goes far beyond that.
country differently, yet hits everyone across the globe. The study was heavily covered primarily for how it debunks Big Alcohol’s pet dissemblance surrounding “healthy alcohol”. As significant as that finding is, however, the significance of the GBD findings goes far beyond that.
Q: What is special about the Global Burden of Disease’s report on alcohol?
GBD’s mission is to provide global contexts for health problems, allowing decision-makers at national and international levels to approach health promotion from an evidence-based perspective. Although alcohol’s health effects are frequently studied, they are often studied region-by-region and outcome-by-outcome. So, for instance, one study might look at cirrhosis and liver cancers in California, while another would look at motor vehicle crashes in Rio de Janeiro. GBD takes over 500 data sets from all over the world combines them into a meta-analysis, tracking 23 different harm outcomes and getting us closer to seeing all alcohol harms in every nation.
Q: What did the study find?
First and foremost, the study found that the only level of healthy drinking is no drinking. This flies in the face of the j-curve hypothesis, which holds that “moderate” drinkers are actually healthier than non-drinkers, and that the only real harm is from drinking too much. So compelling is this hypothesis that Big Alcohol actually managed to scam the National Institutes of Health into running a pet study from a pet investigator intended to demonstrate that alcohol could be medicallyrecommended to people. However, those studies have always relied on only a handful of outcomes related to cardiovascular disease, and be biased in design.
By looking at all outcomes and across all drinkers worldwide, it became apparent that the j-curve was hard to detect and only showed up in a small population subset when it showed up. What’s more, the fleeting cardiovascular effect was drowned out by the other harms—motor vehicle crashes, liver disease and cirrhosis, self-injury, and the increasingly recognized threat of cancer. Ultimately, no drinking could be considered healthy.
- Other significant global findings:
• Alcohol use is the leading preventable cause of death among adults ages 15 to 49
o 3.8% of all mortality in women
o 12.2% of all mortality in men
• Wealthier and more educated countries drink more
o Drinking prevalence in high-income countries, 72% of women, 83% of men
o Daily consumption in high-income countries: 1.9 standard drinks for women, 2.9 for men
• Alcohol is a strong risk factor for tuberculosis
o 1.4% of alcohol-attributable deaths in 15 to 49-year-olds attributed to tuberculuosis
o 1.2% of alcohol-attributable deaths in 15 to 49-year-olds attributed to road injuries
o 1.1% of alcohol-attributable deaths in 15 to 49-year-olds attributed to self-harm
• For women 50 and older, 27.1% of alcohol-related deaths were from cancer
• For men 50 and older, 18.9% of alcohol-related deaths were from cancer
With all that in mind, it is difficult to see claims of alcohol’s healthfulness as anything but a marketing stunt. (That hasn’t stopped Big Alcohol’s proxies from stridently assuring everyone they can keep on drinking, you’re fine, the problem is only those alcoholic over there.) The GBD project is a sorely needed step away from the industry-sponsored conflicting advice meant to keep individuals drinking and towards a single, distilled message for national policymakers: take alcohol use seriously and save your residents’ lives.
Help us hold Big Alcohol accountable for the harm its products cause.
| GET ACTION ALERTS AND eNEWS |
STAY CONNECTED    |
CONTACT US 24 Belvedere St. San Rafael, CA 94901 415-456-5692 |
SUPPORT US Terms of Service & Privacy Policy |